Preventing pressure injuries
What is a pressure injury?
Pressure injuries, also known as pressure ulcers, bed sores or pressure sores, are blisters or breaks in the skin due to ongoing pressure. Pressure injuries, depending on the size, may take a long time to heal, may become infected, may reduce mobility, may leave a scar and can cause great discomfort and pain.
How do you get a pressure injury?
Pressure injuries develop if an area of skin is exposed to constant, unrelieved pressure, from friction which may be caused by moving your body across the bed using heels and elbows or prolonged exposure to moisture.
Who is at risk?
Anyone can develop a pressure injury. You may be more at risk though if you are elderly, frail or have any of the following:
- decreased fluid intake
- confined to a bed and have the inability to move freely
- poor diet
- diabetes, poor circulation or a condition that impairs sensation
- history of smoking
- recent weight loss (without trying)
- loss of bladder or bowel control
- scarred or frail skin or have had a history of pressure injuries.
Where do pressure injuries occur?
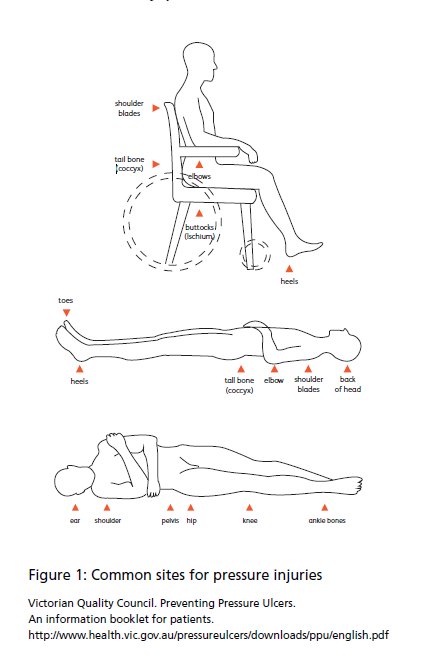
Pressure injuries usually develop over bony areas, especially the buttocks, tail bone, heels, elbows, and hips. Refer to Figure 1 for common locations. Pressure injuries may also develop under medical devices such as stockings or bandages.
Signs to look for:
- Changes in skin colour—may become red, blue or purple.
- Changes in the temperature of the skin— may be cooler or warmer than surrounding skin.
- Changes to the skin surface—may be blistered, swollen, have calluses, shiny areas or dry patches.
What you can do to prevent pressure injuries:
- Inform the nurse caring for you of any painful or reddened areas that may develop.
- Change position regularly, at least every one to two hours.
- If you are unable to reposition by yourself ask staff to assist you.
- Don’t drag yourself up the bed.
- If able, get up frequently and move about.
- Notify the nurse caring for you if any medical devices such as stockings or bandages that are causing you discomfort.
- Don’t massage or rub the skin as this may cause damage to underlying skin tissue.
- Let the nurse caring for you know if you have any damp bedding or clothes.
- Use a protective cream on the skin.
- Stay hydrated and eat a balanced diet.
What your nurse is doing to prevent pressure injuries:
On admission your nurse will determine your risk of developing a pressure injury.
From this, prevention strategies will be put in place which may include placing a pressure relieving mattress on your bed.
The nurse will assess your skin on admission to identify any areas that may be at risk of developing a pressure injury.
If you have a pre-existing pressure injury a treatment plan will be put in place.
The nurses will reassess your risk of developing a pressure injury on a daily basis. This will include checking your skin.
The nurse will come by regularly to reposition you. It is important to change position even if you are comfortable, as pressure injuries can develop quickly.
Remember:
- Report any painful or reddened areas to your nurse.
- Report anything that is causing discomfort such as stockings or bandages.
- Change position frequently, every one to two hours if possible.
- Stay hydrated and eat well.
- Report any damp or soiled clothes and linen to the nurses caring for you.
Anyone can develop a pressure injury.
By following some simple steps to reduce your chance of developing a pressure injury, we can assist you to get back on your feet and home to your family and the things you love without delay.
Read this information in other languages
Preventing pressure injuries—Chinese Simplified
Preventing pressure injuries—Chinese Traditional
Preventing pressure injuries—Vietnamese
Mater acknowledges consumer consultation in the development of this patient information.
Mater Doc Num: Pi-CLN-400016
Last modified 20/9/2019.
Consumers were consulted in the development of this patient information.
Last consumer engagement date: 06/1/2016
For further translated health information, you can visit healthtranslations.vic.gov.au/ supported by the Victorian Department of Health and Human Services that offers a range of patient information in multiple languages.