Pregnancy—information for women and families
Introduction
Your body has a great deal to do during pregnancy. Sometimes the changes taking place will cause irritation or discomfort, and on occasions they may seem quite alarming. There is rarely any need for concern but you should mention anything that is worrying you to your doctor or midwife. If you think that something may be seriously wrong, trust your own judgement and get in touch with your doctor or midwife straight away.
Please use the alphabetical information list on the right or the category list below to navigate this section of the website and find the information you need.
Common problems in pregnancy
Anaemia
Anaemia means you have a low level of red blood cells in your body. Your red blood cells carry oxygen to all of the cells in your body, including to the placenta. During pregnancy it is very common for women to become anaemic. Whilst there are many causes of anaemia, the most commonest cause is not having enough iron.
Iron is essential for making red blood cells. During pregnancy, your total blood volume increases significantly; therefore, you need more iron to make more red blood cells. Your growing baby and placenta also require extra iron. Many women become pregnant, without adequate stores of iron to meet the increased demands of their body and their baby, particularly later in pregnancy.
Good dietary sources of iron include red meats, fortified breads and cereals, green leafy vegetables, legumes and some nuts. You can help your body absorb more iron from non-meat sources by including Vitamin C rich foods at the same meal e.g. tomato, capsicum, citrus fruits and kiwifruit.
It can be hard to get enough iron from your diet. An iron supplement could be useful and may be recommended by your dietitian, midwife or doctor.
Backache
During pregnancy ligaments become softer and stretch to prepare you for labour. This can put a strain on the joints of your lower back and pelvis which can cause backache. As your baby grows, the hollow in your lower back may increase and this may also cause backache.
To avoid backache during pregnancy:
- avoid heavy lifting
- bend your knees and keep your back straight when lifting
- carry heavier loads close to your body
- move your feet when turning round to avoid twisting your spine
- wear flat shoes as these allow your weight to be evenly distributed
- work at a surface high enough to prevent you slouching
- try to balance the weight between two bags if you are carrying shopping
- sit with your back straight and well supported.
A firm mattress can help to prevent and relieve backache. If your mattress is too soft, a piece of hard board under it lengthways will make it firmer. Massage can also help, or you might like to try a support corset—these can be prescribed by your doctor. Make sure you get enough rest, particularly later in pregnancy.
If your backache is very painful, a physiotherapy consultation may help. A physiotherapist will be able to give you some advice and suggest some helpful exercises. The use of heat to relieve discomfort is also very useful. To prevent burns, ensure it is not too hot.
Learn more about back care during pregnancy.
Constipation
You may become constipated very early in pregnancy because of the hormonal changes going on in your body, which tend to make your bowel work more sluggishly.
Make sure you include plenty of fibre in your diet through eating foods like wholemeal breads, wholegrain cereals, fruit and vegetables, and pulses such as beans and lentils. Exercise regularly to keep your muscles toned and make sure you drink plenty of water.
Avoid iron tablets if they cause constipation—ask your doctor whether you can manage without them or change to a different type.
If problems persist, a physiotherapy consultation may be beneficial.
Cramp
Cramp is a sudden, sharp pain, usually in your calf muscles or feet. It is most common at night, but the cause is generally unknown. It usually helps if you pull your toes hard up towards your ankle, provide warmth or rub the muscle firmly. Regular, gentle exercise in pregnancy, particularly ankle and leg movements, will improve your circulation and may help to prevent cramp occurring.
Feeling faint
Pregnant women often feel faint. This happens when not enough blood is getting to the brain. If the oxygen level gets too low, you may actually faint. It’s more common in pregnancy because of hormonal changes taking place in your body. You are most likely to feel faint if you stand still for too long or get up too quickly from a chair or hot bath. It often happens when you are lying on your back due to the weight of the uterus.
Try to get up slowly after sitting or lying down.
If you feel faint when standing still, find a seat quickly and the faintness will pass. If it doesn’t, lie down on your side.
If you feel faint while lying on your back, turn on your side. It’s better not to lie flat on your back in later pregnancy or during labour.
Feeling hot
During pregnancy you are likely to feel warmer than normal. This is due to hormonal changes and to an increase in blood supply to the skin. You’re also likely to sweat more.
To stay cool, wear loose clothing made of natural fibres, as these are more absorbent and ‘breathe’ more than synthetic fibres. Keep your room cool consider using an electric fan or an air-conditioner and wash frequently to stay fresh.
Haemorrhoids
Haemorrhoids are swollen veins around the anus which may itch, ache or feel sore or even bleed a little. They can also make opening your bowels uncomfortable or even painful. Haemorrhoids occur in pregnancy because your veins relax under the influence of pregnancy hormones. They usually resolve shortly after delivery.
If you experience haemorrhoids you should:
- increase your intake of dietary fibre, such as wholegrain bread, fruit and vegetables
- drink plenty of water—this will help prevent constipation, which can make haemorrhoids worse
- avoid standing for long periods
- do regular exercise to improve your circulation
- use an ice pack to ease discomfort, holding this gently against the haemorrhoids, or use a cloth wrung out in iced water
- push any haemorrhoids which stick out gently back inside using a lubricating jelly
- ask your doctor, midwife or pharmacist if they can suggest a suitable ointment
- consider giving birth in a position where the pressure on your anus is reduced—kneeling, for example.
Headaches
Some pregnant women find they get a lot of headaches due to the elevation in pregnancy hormones. A brisk walk may be all you need, as well as a little more regular rest and relaxation. Although it is wise to avoid drugs in pregnancy, an occasional paracetamol tablet is considered safe. If you often have bad headaches, tell your doctor or midwife so that they can advise you. Severe headaches may be a sign of high blood pressure, and you should inform your GP, midwife or obstetrician, who may order further investigation.
Indigestion and heartburn
Many women start getting heartburn and indigestion in the second half of their pregnancy. The burning sensation that is associated with heartburn often extends from the lower throat to the bottom of your breastbone. It usually comes and goes until your baby is born.
Heartburn is caused by both hormonal and physical changes to your body. During pregnancy, the placenta produces the hormone progesterone, which relaxes the smooth muscles of the uterus. Progesterone also relaxes the valve that separates the oesophagus from the stomach, allowing gastric acids to seep back up the oesophagus, which causes that uncomfortable sensation of heartburn. The hormone also slows the wavelike contractions of the stomach, making digestion sluggish. As time goes on in your pregnancy, your baby crowds the abdominal cavity, slowing the emptying of your stomach and pushing up the stomach acids into your throat.
If you suffer from indigestion:
- try eating smaller meals more often
- sit up straight when you are eating as this takes the pressure off your stomach
- avoid particular foods which cause trouble, for example fried or highly spiced ones, but make sure you are still eating well.
Heartburn is more than just indigestion. It is a strong, burning pain in the chest. It is caused by the valve between your stomach and oesophagus relaxing in pregnancy, so that stomach acid passes into the oesophagus. It is often brought on by lying flat.
Heartburn can be made worse by:
- tight clothing
- smoking
- stress
- bending down too soon after eating
- slumped sitting posture
Foods that may trigger symptoms and are best to avoid include:
- alcohol
- caffeine (coffee, tea, cola drinks, chocolate)
- spices
- citrus juices, tomatoes and peppermint may cause discomfort in more severe cases.
Other strategies to help avoid heartburn include the following:
- eat small, frequent meals
- eat slowly and chew well
- avoid having late meals, allow two to three hours before going to bed or lying down
- drink fluids in between meals, rather than with them
- elevate the head of the bed (15 to 20 cm) or use pillows to prop up your head
- don’t bend over directly after meals; keep upright.
- sit with good posture, lean back into chair and don’t cross your legs
- try drinking a glass of milk or eating six to seven almonds
- ask your doctor or midwife for advice;
- don’t take antacid tablets or mixture before checking that they are safe in pregnancy.
Itching
Mild itching is common in pregnancy because of the increased blood supply to the skin. In late pregnancy the skin of the abdomen is stretched and this may also cause itchiness. Wearing loose clothing may help.
Itching can, however, be a sign of a more serious problem called obstetric cholestasis. If itching becomes severe; particularly in the palms of your hands and/or the soles of your feet, see your doctor. Itching which is associated with a rash may also need treatment if it is severe.
Ligament pain
Ligament pain can be a sharp pain or a feeling of discomfort in the lower abdomen or the right or left side of your abdomen. It can be quite uncomfortable and is most likely to occur between 16 and 20 weeks. It is a sign that your body is stretching to allow your baby to grow and you should not be alarmed. It is common and normal to have ligament pain in the second trimester.
Nausea and morning sickness
Nausea and vomiting in pregnancy is extremely common and is usually referred to as morning sickness, although the nausea and vomiting can occur at any time of day. Studies estimate that nausea and vomiting occurs in 50 to 90 per cent of pregnancies. For the majority of cases morning sickness is not a serious condition and does not place the mother or baby at risk.
The most severe form of nausea and vomiting in pregnancy is called hyperemesis gravidarum. This condition can place the mother and baby at risk because the nausea and vomiting prevent the mother form retaining and utilising food and fluid. This occurs in approximately one per cent of pregnant women and can start between four to six weeks of pregnancy. Symptoms usually resolve from about 15 to 20 weeks but occasionally last the whole pregnancy.
Learn more about morning sickness and hyperemesis gravidarum.
Nose bleeds
Nose bleeds are quite common in pregnancy because of hormonal changes and while usually short in duration can be quite heavy. To help the bleeding stop, press the sides of your nose together between your thumb and forefinger just below the bony part of your nose for ten minutes. Repeat for a further ten minutes if this is unsuccessful. As long as you don’t lose a lot of blood, there is nothing to worry about. Blow your nose gently and try to avoid explosive sneezes. You may also find that your nose gets more blocked up than usual. You should inform your GP, midwife or obstetrician if the nose bleeds persist as further investigations may be required.
Passing urine often
Needing to pass urine often is an early sign of pregnancy. Sometimes it continues right through pregnancy. In later pregnancy it is the result of your baby’s head pressing on your bladder. If you find that you have to get up in the night, you could try cutting out drinks in the late evening but make sure you keep drinking plenty during the day. Later in pregnancy, some women find it helps to rock backwards and forwards while they are on the toilet. This lessens the pressure of the uterus on the bladder so that you can empty it properly and you may not need to pass urine again quite so soon.
If you have any pain while passing urine, or pass any blood, you may have a urinary tract infection which will need treatment. Drink plenty of water to dilute your urine and reduce any irritation. You should contact your General Practitioner within 24 hours.
Sometimes pregnant women are unable to prevent a sudden spurt of urine or a small leak when they cough, sneeze or laugh, or when moving suddenly or just getting up from a sitting position. This may be temporary because the pelvic floor muscles relax slightly to prepare for your baby’s birth and your growing baby will increase pressure on the bladder. If you find this a problem, you can improve the situation by doing exercises to tone up your pelvic floor muscles. Ask a midwife or physiotherapist for advice. Pelvic floor exercises should be exercises for life.
Skin and hair changes
Hormonal changes taking place in pregnancy may make your nipples and the area around them go darker. Your skin colour may also darken a little, either in patches or all over. Birthmarks, moles and freckles may also darken. Some women develop a dark line down the middle of their stomachs. These changes will gradually fade after your baby has been born, although your nipples may remain a little darker.
If you sunbathe while you are pregnant, you may find you tan more easily. Protect your skin with a good, high-factor sunscreen and do not stay in the sun for very long.
Hair growth is also likely to increase in pregnancy. Your hair may also be greasier. After your baby is born, it may seem as if you’re losing a lot of hair. In fact, you’re simply losing the increase in hair that occurred during pregnancy.
Sleeplessness
Late in pregnancy it can be very difficult to get a good night’s sleep. You’re uncomfortable lying down, or just when you’re beginning to get comfortable, you have to get up to go to the toilet. Some women also have strange dreams or nightmares about their baby and about the birth—talking about them can help you. The relaxation and breathing which are taught in antenatal classes can be helpful.
Stretch marks
These are pink or purplish lines which usually occur on the tummy or hips and sometimes on the upper thighs or breasts. Some women get them, some don’t. It depends on your skin type. Some people’s skin is more elastic. You are more likely to get stretch marks if your weight gain is greater than average. After your baby is born, the marks should gradually pale and become less noticeable. It is very doubtful whether oils or creams actually help prevent stretch marks.
Swollen ankles, feet and fingers
Ankles, feet and fingers often swell a little in pregnancy because the body holds more water than usual. Towards the end of the day, especially if the weather is hot or if you have been standing a lot, the extra water tends to gather in the lowest parts of the body.
You should:
- try to avoid standing for long periods
- wear comfortable shoes
- put your feet up as much as you can
- try to rest for an hour a day with your feet elevated.
Teeth and gums
Bleeding gums are caused by a build-up of plaque (bacteria) on the teeth. During pregnancy, hormonal changes in your body can cause the plaque to make the gums more inflamed. They may become swollen and bleed more easily.
To keep your teeth and gums healthy, you should:
- pay special attention to cleaning your teeth. Ask your dentist to show you a good brushing method to remove all the plaque
- avoid having sugary drinks and foods too often. Try to keep them only to meal times,
- discuss with your dentist whether any new or replacement fillings should be delayed until after your baby is born.
Vaginal discharge
Almost all women have more vaginal discharge in pregnancy. It should be clear and white and it should not smell unpleasant. If the discharge is coloured or smells strange, or if you feel itchy or sore, you may have a vaginal infection. Tell your doctor or midwife. The most common infection in pregnancy is thrush, which can be treated easily. You can help prevent thrush by wearing loose cotton underwear as well as avoiding perfumed/scented soaps, shower gels and bubble baths if you are susceptible to vaginal thrush infection. If vaginal discharge, of any colour, increases a lot in later pregnancy, tell your doctor or midwife.
Varicose veins
Varicose veins are veins which have become swollen. The veins in the legs are most commonly affected. You can also get varicose veins in the vulva (vaginal opening). They usually improve after the birth of your baby.
You should:
- try to avoid standing for long periods of time
- try not to sit with your legs crossed
- try not to put on too much weight as this increases the pressure
- sit with your legs up as often as you can to ease the discomfort
- try support stockings, which may also help support the muscles of your legs—you can buy them at most pharmacies
- try sleeping with your legs higher than the rest of your body—use pillows under your ankles or put bricks or books under the foot of your bed
- exercise such as walking, cycling and swimming, which will help your circulation,
- massage your legs in an upward movement.
More serious problems
Slow-growing babies
Many of the tests in pregnancy check the growth of your baby. If you have previously had a very small baby, or if you smoke heavily, the midwives and doctors will monitor your pregnancy closely. If there is concern about your baby’s health, further tests may be carried out and more frequent monitoring of your baby may be recommended.
In the last weeks of pregnancy you may also be asked to keep track of your baby’s movements. If you notice your baby’s movements becoming less frequent or slowing down, or if they stop, contact your midwife or doctor immediately. If tests show that your baby is not growing well in the womb and your baby is at risk, early delivery by induction of labour or caesarean birth may be recommended.
High blood pressure and pre-eclampsia
During pregnancy your blood pressure will be checked at every antenatal appointment. High blood pressure is one of the most common medical problems of pregnancy.
Learn more about high blood pressure in pregnancy.
Vaginal bleeding
Bleeding from the vagina at any time in pregnancy may be a concern. In early pregnancy, bleeding may be a sign of an ectopic pregnancy or a miscarriage, however many women who bleed at this time go on to have normal and successful pregnancies. If you have bleeding with pain, contact your obstetrician or the hospital straight away. You may be referred to the Pregnancy Assessment Centre (PAC) which is a specialist area in the Mater Mother’ Hospitals that deals specifically with problems in early pregnancy, 24 hours a day.
Learn more about the Mater Mothers’ Hospitals Pregnancy Assessment Centre.
Bleeding after 20 weeks of pregnancy may be caused by cervical ectropion, vaginal infection, placental edge bleed, placenta praevia or placental abruption.
Learn more about antepartum haemorrhage – bleeding in pregnancy.
The most common sort of bleeding in late pregnancy is the small amount of blood mixed with mucus, known as a ‘show’. This is a sign that the cervix is changing and becoming ready for labour to start. It may happen a few days or a week before contractions start or during labour.
Deep vein thrombosis (DVT)
DVT is a serious condition where clots develop, often in the deep veins of the legs and can be fatal if the clot travels from the legs to the lungs. Flights over five hours, where you sit still for a long time, may increase the risk of DVT. Pregnant women and women who have recently had a baby are among those more at risk. If you intend to travel by air, consult your midwife or obstetrician before the trip. Get advice on in-seat exercises to keep your circulation active. After the 28th week of pregnancy, most airlines require a letter from your obstetrician to say that you are fit to travel. If you develop swollen painful legs or have breathing difficulties after the trip, contact your obstetrician or go to your nearest Emergency Department immediately.
Physical changes during pregnancy
Your changing body
Pregnancy causes your body to change as hormones soften the supporting ligaments and muscles. As your baby grows, extra strains are placed on your body—your spinal curves, muscles and ligaments.
Using regular and gentle (low impact) exercise is a great way to maintain your fitness, reduce stress, decrease fatigue and keep healthy throughout your pregnancy. Always wear good arch-supportive shoes, particularly while you are exercising, as it can help reduce stresses and strains on your body and also assists in maintaining good posture.
Posture
It is important to think about good posture not only while exercising but also in everyday situations. If you avoid movement combinations such as bending and twisting you can help prevent back injury. Drawing in your pelvic floor muscles and gently “bracing” before and during any kind of moving activity you will protect your back, pelvis and pelvic organs. Pelvic floor exercises before and after the birth of your baby are a good way to help keep your muscles strong and will help promote a faster recovery.
A helpful way to think about good posture is to stand up as tall as possible, letting your shoulders relax down. It’s a good idea to avoid standing on just one leg, or any kind of slouched position as this can place strain on your back and other joints in your body. Other potential strains can be prevented by not lifting or carrying heavy loads such as toddlers or groceries. Make use of strollers or ask for help with activities around the home. Think about maintaining good posture while cooking and performing other daily activities.
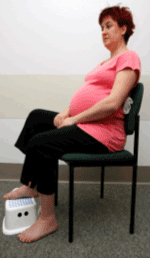 Good posture is also important when you’re sitting, whether on the lounge, in the car, at the computer or in the future when feeding your baby. When sitting in a chair, keep your back well supported by placing your bottom well back in the chair and leaning back to the chair, not slouching forwards. Think about your weight being taken evenly on your thighs rather than your tailbone. To maintain good sitting posture don’t cross your legs. For better support, you can place a small rolled towel in the curve of your lower back, or place one foot on a footstool.
Good posture is also important when you’re sitting, whether on the lounge, in the car, at the computer or in the future when feeding your baby. When sitting in a chair, keep your back well supported by placing your bottom well back in the chair and leaning back to the chair, not slouching forwards. Think about your weight being taken evenly on your thighs rather than your tailbone. To maintain good sitting posture don’t cross your legs. For better support, you can place a small rolled towel in the curve of your lower back, or place one foot on a footstool.
Getting comfortable
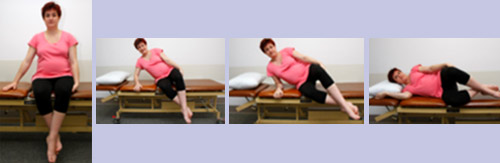
Try different resting positions using furniture, pillows and other supports to relieve any joint aches and to support the weight of your baby, but avoid lying flat on your back.
Ideally you want to keep your body straight and avoid any twisted positions. When you’re lying down, a side lying position with a big pillow or beanbag between your legs for support will help take any strain off your back and legs.
This keeps your top leg in a bent ‘open’ position and also helps your body remain straight. If you’re standing and experiencing backache, you can help relieve this by leaning forward and putting your weight through your arms using different available supports such as your shopping trolley, benches, or support people. It’s good to avoid long periods of standing, but if you have to stand for a length of time (e.g. when ironing or washing dishes), you can adjust your position by stepping one foot up on a phonebook for example, or perhaps using the ledge under the kitchen sink.
Try to avoid squatting as this can place unnecessary strain on your body. Experiment with different kneeling and half-kneeling positions or use a small stool to sit on.
Back care during pregnancy
Avoiding bending and lifting is one of the best ways to prevent back strain, however when you do need to lift, it’s important to use safe bending and lifting techniques. Always position yourself close to the object you are lifting, and gently “brace” by drawing in your pelvic floor muscles before and while you are lifting.
Bending forwards by using your hips and knees, always keep your back straight while maintaining the natural curve in your low back. Be sure to avoid any twisting movements and as you come up, allow your legs to do the work, keeping your back in its safe position. Always keep breathing and moving smoothly to help protect your spine and pelvic joints.
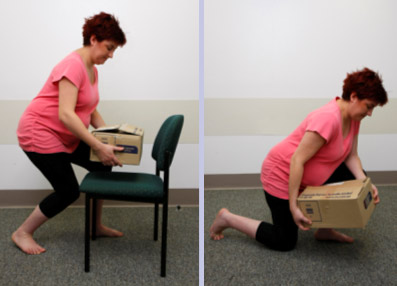
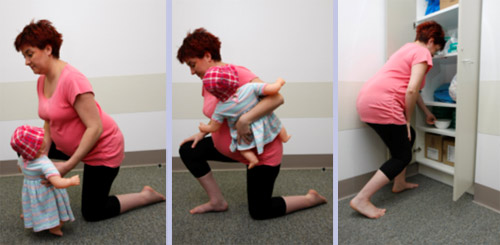
Gentle stretches can prevent or ease backache
During any kind of movement, always listen to your body and ensure you’re not experiencing any pain. If you do experience pain, try modifying your position. Never ‘push through’ pain at any point. All movement should be performed smoothly and comfortably, without holding your breath or straining. Performing gentle stretches can help improve circulation and relieve tired muscles.
These stretches can include:

- kneeling squarely on your hands and knees, tucking your head and chin under your chest, tuck your bottom under as you arch your central back up smoothly. Pause, then release. Repeat several times
- slowly moving your pelvis around in a circular motion. You can do this in standing or on all fours.
Exercising too vigorously or performing ‘sit-up’ movements should be avoided at all times. If you become aware of a central ridge appearing in your tummy while exercising, contact your physiotherapist.
Getting out of bed
You can protect your back and tummy by getting into and out of bed with minimal strain. As you get out of bed, this is done by bending your knees up one at a time and keeping them bent while you roll onto your side. Make sure you are not too close to the edge of the bed before you use your strong arms to push yourself forwards and up from your side. Your legs stay bent throughout the movement and should pivot downwards simultaneously as you push forward and up.
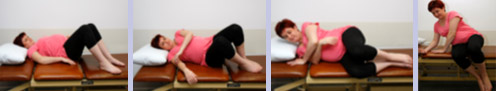
Getting into bed
To protect your back and tummy getting back into bed, sit down on the bed with your bottom well back on the bed (your feet might be off the floor). If you cross your ankles and grasp under the top thigh, this will assist. As you lower yourself down onto your side, keeping your hips and knees bent, your lower legs pivot up as your feet tuck up underneath your bottom.
Getting in and out of bed without straining your tummy—ALWAYS the best way to do it!
Pelvic floor muscles
The pelvic floor is made up of a sling of muscles and tissue. They stretch like a hammock from the pubic bone at the front to the tailbone at the back. The three openings (urethra, vagina and rectum) pass through the pelvic floor muscles. Strong pelvic floor muscles prevent leaking of urine, wind and faeces. They also play a part in sexual function and stability of the spine. Strengthening your pelvic floor muscles is important before and after the birth of your baby. By practising strengthening exercises regularly you can help ensure these muscles stay strong.
To activate and strengthen your pelvic floor muscles, position yourself by either sitting up tall or lying on your side. You should feel comfortable in whichever position you choose, with your back in a “neutral” curve and your tummy, buttocks and thighs fully relaxed.
Gently draw your pelvic floor muscles up in a “squeeze and lift” action by imagining you are stopping the flow of urine. At the same time continue to breathe easily. This will close off and draw up the muscles around your front passage, vagina and back passage. Aim to hold this contraction for up to 10 seconds, and then relax for 5 seconds.
Make sure you’re not squeezing your buttocks or bearing down or straining in any way. Repeat this action up to 10 times. You can further progress to performing 10 short, fast, and strong contractions.
Performing this set of exercises three times daily will help you to maintain good bladder control, or help improve your control of your bladder if you find urgency or frequency is a problem.
It is a good idea to “brace” with these muscles before you lift, move, cough, laugh or sneeze. If you find you cannot activate these muscles, are holding your breathe or seem to be straining, stop performing the exercise and talk to your physiotherapist. Regular pelvic floor exercise is important in pregnancy, but you need to make sure you are doing the right thing.
Additionally, it’s important to not repeatedly stop the flow of urine mid stream as an exercise as this is not good for your bladder.
Good bowel and bladder habits
 Good bowel and bladder habits include the following:
Good bowel and bladder habits include the following:
- Drink 1.5 to 2 L of fluid each day.
- Empty your bladder up to eight times per day.
- Take your time—don’t hurry or strain to empty bladder or bowel.
- Sit properly on the toilet—don’t hover, always use the defaecation position—see image to the right.
- Maintain bladder capacity—no ‘just in case visits’ to the toilet.
- Have strong pelvic floor muscles. Exercise three sessions each day and ‘brace’ them before and as you move.
Maintain your fitness with regular, gentle exercise
It’s important to maintain your fitness with regular, gentle exercise throughout your pregnancy. Exercise programs that include walking or aqua aerobics are ideal. Utilise the pelvic floor “bracing” technique to protect your body throughout each exercise session. You are free to continue with your regular non-contact sports for as long as you are comfortable doing so. However, if you are experiencing any pain or discomfort in any exercise activity, be sure to stop the activity and seek professional advice. Starting new sports or participating in vigorous exercise should be avoided while you are pregnant. Contact sports especially should be avoided, particularly after you are four months pregnant.
Guidelines for exercising safely
- Exercise safely in specially designed classes.
- Get your doctor’s okay.
- Avoid exercising in the heat and for prolonged periods.
- Eat an hour before exercising.
- Drink plenty of water before, during and after exercising.
- Go to the toilet before beginning exercising.
- Begin with warm-up—large, free body movement and stretches.
- Finish with a slow cool-down including stretches.
- Always get up slowly when rising from the floor.
- Don’t push through any pain or discomfort—use alternate exercise.
- Exercise at your own pace—rest if tired or short of breath.
- You should be able to maintain a conversation as you exercise i.e. NOT short of breath.
- Never exceed heart rate of 140 beats per minute, or less if advised by your doctor, or have slow resting heart rate.
- Wear cool, comfortable, supportive clothes that allow freedom of movement. Bike pants or tights, a good bra and sports shoes to support the arches of the feet are recommended.
Avoid:
- spending any time on your back
- any sit-up or abdominal crunch exercises while pregnant
- rapid alternating movements
- any high impact activities.
Seek further help from the physiotherapist if you experience any of the following:
- Pelvic joint pain—pubic symphysis or sacro-iliac joint (SIJ) or sciatica Grinding/grating, severe aching, sudden stabbing pain, unable to take weight, limping, muscle spasm, “sciatica”, pain on movement including walking, pain on lifting one foot up such as putting shoes or underwear on.
- Rectus diastasis—separation of the abdominal muscles. A bulge appears in the central line of the abdomen as you get up, change position, lift, cough, etc. To help avoid this, make sure you lie fully on your side before you get out of bed, and NO sit-ups.
- Lower back, thoracic (mid back) or neck pain.
- Bladder control problems—accidental loss of urine with cough, sneeze, or movements or bladder urgency or frequency.
- Problems with constipation and/or straining to empty the bowels.
- Carpal tunnel syndrome—numbness, pins and needles, tingling or pain in the fingers and hand or wrist.
- Localised muscle tension or cramps.
Physical relaxation during pregnancy
Being able to relax is a valuable skill for normal labour and in everyday life; however relaxation is a skill that requires practice. If you start to practise relaxation techniques regularly, at least once a day, you will start to notice an improvement in your energy levels and an improved ability to cope with potentially stressful situations.
Start your practise in quiet surroundings with minimal distractions. Ensure you are comfortable and in a well-supported position, and then allow yourself to focus on your breathing. Inhale with a gentle relaxed breath, and then follow by focussing on your outward cleansing breath, as you allow for a release of any tension from your body.
Breathing as slowly as is comfortable and as low down in your lungs as you can gives you a central focus and promotes an even rhythm of breathing. This reduces the feelings of panic, from breathing too high and fast, and allows your body’s natural endorphins to be released. If you have practised and can apply the skills of physical relaxation, especially your “trigger points” during contractions, you will conserve enormous amounts of energy and feel much more in control of your body.
Allow yourself 20 minutes for relaxation sessions initially. With practise you will be able to decrease the amount of time it takes for you to relax, and also be able to practice in less quiet surroundings. By practising regularly, you will eventually find you have the ability to become relaxed simply by taking one breath in followed by a cleansing breath out, regardless of external distractions.
Relaxation instructions
Sit or lie in a comfortable, supported position, become aware of your body as you start to tune-in:
- Focus on the easy, gentle rhythm of your normal breathing pattern:
- allow your body to become loose and heavy
- with each breath out—let go a little bit more.
- Pull your feet up towards you—hold:
- stop pulling
- let them hang heavily.
- Move your knees slightly apart—hold the thigh muscles tense:
- stop holding
- let them rest comfortably.
- Tighten your buttocks, thighs and pelvic floor—hold:
- release tension
- feel the softness.
- Feel the easy rhythm of your breathing-with each breath out, let go a little bit more.
- Stretch your fingers and thumb out straight—hold:
- stop stretching
- feel the “slackness” in your hands.
- Pull your shoulders down towards your waist—hold:
- stop pulling
- now feel the looseness around your shoulders and neck.
- Raise your eyebrows and keep them up:
- stop lifting them
- be aware of the tension fading out of your forehead.
- Now gently lower your eyelids if your eyes are not already closed:
- underneath, your eyes should feel heavy and be still.
- Open your mouth wide—pull your chin down:
- stop pulling
- your lips will be soft, your teeth slightly apart, your tongue resting loosely in your mouth
- be aware of how warm and soft your face is.
- Focus again on your slow, easy breathing, with each breath out, let go a little bit more.
- Now allow yourself time to enjoy this wonderful state of relaxation—perhaps try some visualisation techniques.
Feelings and emotions
From the minute you know you are pregnant, things begin to change—feelings about yourself, about your baby, about your future. Your relationships change—with your partner, other children and also with parents and friends. Adjusting to the changes that pregnancy brings isn’t always easy.
Emotions
Most women experience a range of different emotions from the time they find out they are pregnant through to and after birth. In the first few months there is often a mixture of happiness and excitement, and for some dismay, verses worry about the changes a baby will bring in relationships, roles and finances as well as the worry about the health of the baby and the ability to parent.
Many women will feel teary and irritable in addition to the physical problems of fatigue and morning sickness. For some this can be very different to how they expected to feel. This wide range of experiences is common and generally settles as the pregnancy progresses and psychological adjustment occurs. When the pregnancy is unplanned there may be more difficulty in adjusting to the news and the impact the pregnancy brings.
After the first three months of pregnancy, many women start to adjust to the changes, begin to feel physically better and emotionally more stable. There is often a growing sense of attachment to the baby and some easing of worry about the baby’s health.
Many women start to actively plan and prepare for the baby by buying clothing and baby items. As the birth gets closer most women begin to feel more tired and uncomfortable and it is common to worry about the birth. Some women have more difficulty sleeping and have vivid dreams about themselves or their baby.
Some women will enjoy an uneventful pregnancy but for others there are some difficulties along the way. Our emotional and physical health are closely linked so taking care to get adequate sleep and rest, eating well and having regular antenatal care can have positive emotional benefits. Learning about pregnancy, the expected changes, labour and parenting is also helpful and can be done by reading, talking with family and friends and attending antenatal classes.
Attend to your important relationships and try and minimise the stress where possible in your life. Consider the ways you usually cope with stress and whether there are new skills you could learn such as problem solving, time management and relaxation. Look at your available supports e.g. women’s groups, social groups, mothers’ groups and playgroups.
Birth Anxiety
One of the most common concerns that women have during pregnancy involves the pain associated with labour and child birth and how they will cope. The experience is different for every woman, however information about the options open to you can help you feel more confident and in control.
Below are just a few of the ways of managing and hopefully decreasing the worries about the birth of your child:
- Ask your midwife or obstetrician for further information.
- Antenatal classes are a good way to help you prepare for your labour and birth.
- Think about the sort of labour and birth you would like to have. You can discuss these possibilities in more detail with your midwife, obstetrician and support people and draw up a birth plan. Birth plans should be discussed with your midwife or obstetrician during your pregnancy.
- Talk to your partner, as well as your chosen support person who will be with you in labour.
- No matter how much you plan for your birth, surprises may occur. While you cannot guarantee an easy birth, taking the above steps can help to reduce some of the stress that accompanies pregnancy.
Worrying about abnormality
There is some stage during every pregnancy when people worry that there may be something wrong with their baby. There are a number of ways of coping with this possibility, all of which are understandable. Talking openly about abnormality and refusing to dwell on it are two very different, but very common ways of dealing with the anxiety that something might be wrong with a pregnancy.
Only a small proportion of babies are born with abnormalities, with the vast majority being born healthy. Much of the time, these abnormalities can be detected antenatally and support can be put in place for when it is time for your baby to go home. If you are feeling particularly anxious or concerned about the possibility of your baby having an abnormality, talk to your obstetrician or midwife as soon as possible. They can discuss the risks with you and provide you with opportunities to make informed choices. They can also refer you on to a social worker, who can assist with strategies to decrease anxiety and can provide support around postnatal planning if there is a problem with your pregnancy.
Relationships
Pregnancy is bound to bring about some quite significant changes in a couple’s relationship, especially if this is your first baby. For some people these changes happen easily, while others find it harder to change. Everybody is different.
It’s quite common for couples to find themselves having arguments every now and then during pregnancy, no matter how much they are looking forward to the baby. Some of these may be nothing to do with the pregnancy, but others may be caused by one or the other feeling worried about the future and how they are going to cope. Perhaps the most important thing to realise is that during pregnancy there are understandable reasons for the unusual difficulty between you and also good reasons for feeling closer and more loving. One practical question you will need to discuss is how you will cope with labour and whether your partner will be there. Many partners want to be present at their baby’s birth.
Sex in pregnancy
Many people worry about whether it is safe to have sex during pregnancy. There is no physical reason why you shouldn’t continue to have sexual intercourse right through a normal pregnancy, if you wish. It doesn’t harm your baby because the penis cannot penetrate beyond the vagina. The muscles of the cervix and a plug of mucus, specially formed in pregnancy, seal off the uterus completely.
Later in pregnancy, an orgasm, or even sexual intercourse itself, can set off Braxton Hicks’ contractions. You will feel the muscles of your uterus go hard. There is no need for alarm as this is perfectly normal. If it feels uncomfortable, try your relaxation techniques or just lie quietly till the contractions pass. Your obstetrician or midwife will probably advise you to avoid intercourse if you have had heavy bleeding in pregnancy, and you should definitely not have intercourse once your waters have broken, as this increases the risk for infection to your baby. While sex is safe for most couples in pregnancy, it may not be all that easy. You will probably need to experiment with different positions.
Some couples find making love extra enjoyable during pregnancy while others simply feel that they don’t want to have intercourse and prefer to find other ways of being loving or of making love. It’s important to talk about your feelings with each other.
Family support
Having the support of your partner, family and friends can be very helpful during pregnancy. However, it may also be very stressful. Pregnancy will have a profound impact upon the relationships that you have with the people closest to you. The changes brought about by a new arrival can put stress on these relationships and it can take some time to adjust to this period of your life.
You may find that the connection you have with your partner is the first to change. This will impact on each person’s life significantly as your outlooks, lifestyles and priorities are thrown up in the air. Couples dealing with these adjustments sometimes adapt very easily, but it is quite normal to struggle and arguing more often is one way many couples deal with this upheaval. Arguments can be about anything, from concerns about the birth and the future in general to issues that appear completely unrelated to the pregnancy. The majority of these conflicts can be traced back to simple anxiety about parenthood, but it is important to remember that like you, your partner may also be scared and worried about how to cope with having a baby.
Family and friends can provide a great deal of help and support in many different ways, not only during your pregnancy, but also after you take your baby home. A support network of family and friends can provide emotional support e.g. advice or someone to just talk through your worries with, as well as practical assistance e.g. child care or transport to appointments.
However, this support can, sometimes, become too much. People may become overbearing with the involvement they wish to take in your life. They can give you advice you do not want or need; they can expect to be informed about every change in the pregnancy, and they can even become critical of the decisions that you are making. It is essential to maintain some boundaries during your pregnancy and to try to be assertive in enforcing these boundaries. It may be helpful to gently explain to family and friends that there are some decisions that only you and your partner can make. You are the ones going to be parents and you need to decide what is right for you and your baby.
Coping alone
Being pregnant and single can be a challenging and scary prospect, but having a good support network can greatly reduce the amount of stress and anxiety you may experience throughout your pregnancy. Talk to your friends and family, as they may be able to help, both practically and emotionally.
If you have limited family support, there are a number of organisations in the community who can provide assistance in a short and long term capacity. Financially, you can access Centrelink for a number of different entitlements both antenatally and after the birth of your baby. A range of income support options and one off payments are available depending on your family's financial situation. Please visit the Centrelink website for further information or visit your local Centrelink office.
If you are concerned about whether you will be able to cope as a single mother, please talk to your obstetrician or midwife. They can refer you to a social worker, who will be able to link you up with different services and community centres that may meet your needs.
Work
Many women have mixed feelings when it comes time to stop work to have a baby. Giving up that part of your life can take some adjusting to and you should spend some time dealing with this change in your own way. There are a number of ways to spend this time before the birth. Some women find it a good time to just relax and enjoy setting up their baby’s room. Others use the time to expand their social networks by joining a mothers’ group or a playgroup. Each woman is different and you will probably have your own plans for this short period.
Returning to work is also something that is different for everyone. You may wish to spend a long time at home with your baby, or you may need to return to work, either full or part time, fairly soon after the birth. You may also decide to not return to work and become a stay at home mother. These are all valid choices to make, but there are certain steps that need to be taken if you do choose to return to work. The highest priority is determining child care for your baby. You may be able to organise for your partner, family or friends to care for your child while at work, however if this is not an option it will be necessary to investigate other childcare arrangements. Childcare centres attract a high demand, so it is wise to book in early in your pregnancy if you wish to obtain a place. Some community centres and organisations such as Family Day Care also provide childcare, but again it is important to be organised if attempting to access these services.
Domestic violence
About 15 per cent of all women have experienced domestic violence at some point in their lives. Domestic violence has many forms. Among these are physical and sexual violence, emotional and social abuse e.g. preventing contact with friends or family, and economic deprivation e.g. withholding money. Contrary to what many people think, the risk of domestic violence during pregnancy actually increases. Statistics show that of the women who had experienced violence by a previous partner 36 per cent reported that the violence occurred during pregnancy and 17 per cent stated the violence had occurred for the first time during the pregnancy.
Domestic violence is something that you should not have to live with at any time of your life. Pregnancy is a high risk time and with the increased stress it puts on relationships, domestic violence can occur. If you think you might be in a relationship where this is occurring, or if you feel afraid for your own safety, you should contact a social worker, obstetrician or midwife at the hospital, or one of the organisations listed below. They can help you to take steps to stop the violence or to escape the situation.
Support services
Mental health issues during pregnancy
For some women the adjustment to being pregnant may be more difficult and they may worry because they feel different to how they expected. If you are concerned or notice changes in your feelings that persist, or affect your functioning, it is important to talk with your obstetrician, midwife or General Practitioner.
Mental health problems are common in pregnancy. It is a time when women are more vulnerable to psychological distress and mental illness such as depression or anxiety. Women with a previous personal or family history of depression or mental illness are at greater risk of depression in the antenatal or postnatal period. For women with a history of depression or other mental illness, it is advisable that they have an assessment for depression early in their antenatal period with their doctor or midwife. Other factors that may be risk factors are an unplanned pregnancy, difficult or complicated pregnancy, being single or having inadequate partner support, domestic violence, and drug and or alcohol misuse.
About 13 per cent of women will experience depression during pregnancy, called antenatal depression, and if untreated this can have negative outcomes for both mother and baby and continue into the postnatal period. The common symptoms of depression are feeling depressed or anxious most of the time, poor appetite, difficulty sleeping, and lack of concentration, motivation and enjoyment. In severe depression people have feelings of hopelessness, worthlessness and suicidal ideas. Depression is very treatable if detected.
The Edinburgh Depression Scale is routinely used at Mater Mothers’ Hospitals and consists of a number of questions that can help identify women who may have depression or anxiety. When you complete these questions the midwife will score the answers and for women scoring twelve or more, recommend an assessment either with their local doctor or a mental health specialist. This assessment can determine if a woman is suffering from depression, anxiety or other mental health condition, and then appropriate help can be organised.
Encouraging good mental health in pregnancy
Good mental health in pregnancy can be helped by a number of strategies including:
- good nutrition
- reducing or stopping alcohol and or drug use
- regular antenatal care
- gaining information about pregnancy
- regular exercise appropriate to pregnancy
- use of relaxation and anxiety management strategies
- broadening of social contacts and supports, particularly in preparation for the postnatal period
- talking about your feelings with your partner, support people or a health professional
Information for fathers
You may experience a huge range of emotions when you find out you will become a father. Feelings of joy and happiness are common, but feelings of anxiety, uncertainty and fear are just as normal.
- Will our baby be healthy?
- Can we cope on one wage? We'll never have any money again.
- Is the house big enough?
- I don't know anything about babies. I won't know what to do.
- Everyone keeps telling me my life is over. I'll never see my mates again.
- How will the pregnancy affect my relationship?
Worries such as these are perfectly normal when you are adjusting to your new role as a father. Some may be well founded, others not. It can be tempting to stay quiet about these anxieties, thinking you do not wish to trouble your partner or that you should not be feeling these things. However, by repressing these thoughts you may actually increase the escalation of fear and worry that you experience.
Make certain that you talk about your anxieties around the pregnancy and relationship changes with your partner. She may very well have the same concerns. Keeping silent can not only increase your worries, it can also exacerbate any uncertainties that she may have. Discuss your expectations with each other. Otherwise, it can be very easy for one or both of you to become isolated, not only from each other, but also from your family and friends. Talking about these things will enable you and your partner to feel more prepared.
Supporting your partner
Becoming a father is one of the most important, difficult and rewarding things you will ever do, and more often than not, it is the role men are least prepared for.
Traditionally, fathers have been responsible for discipline and setting rules in the family, while mothers did most of the caring. Unfortunately, this has led to a belief by many men that women were solely responsible for parenting. Today, there is greater acknowledgement of a father’s role in the pregnancy, birth and parenting of a child, and there is no clear difference between men’s and women’s roles. As a result, it is not uncommon for new fathers’ to feel unsure about what is expected of them.
There is no single recipe for being a father. The reality is that you will learn as you go, getting to know your baby's individual personality and temperament, and doing what's right for you according to your personal, family and cultural circumstances.
While parenting can be done by either parent, children still have different experiences with their fathers than with their mothers. Fathering is not the same as parenting. Children are lucky if they know they are loved and cared for by both parents. Many fathers know what they don’t want to do from memories of their own childhoods, but they aren’t sure what they should do.
How you work it out will depend on:
- what you expect to do as a father
- what your child's mother expects
- what your partner expects if she is not your child's mother
- the way you and your partner balance work and family responsibilities—how you prioritise your children and family
- the good things that you want to keep from what your own father did
- the things that you see other fathers do
- what your own children want and need.
The most important gift you can give your children is your love. This means getting to know them and sharing who you are as a person. It means spending time with them and making the most of that time you spend with them.
The birth of your baby
Most fathers are present at their baby's birth these days. Childbirth can be joyful, unpredictable, exciting, messy, painful, and physically and mentally exhausting. It is important to remember your purpose at the birth is as a support person and advocate for your partner. You are there to help her, to soothe her, to encourage her, to reassure her, and to help her make choices or decisions in childbirth.
To do this, remain calm and controlled. Above all else, be flexible, and be prepared to adapt if things don't go to plan.
The best antidote for fear is facts. Talk to your obstetrician and midwife. Ask questions so you understand what is going on and whether there is anything you can do to help.
Breastfeeding
Breastfeeding has many advantages—to your baby, to your partner and to you. Breast milk contains all the nutrients needed by your baby for the first six months of life, in exactly the right amounts, and remains the most important part of an infant’s diet for twelve months.
Human milk contains antibodies which protect your baby from gastrointestinal and respiratory illnesses. Breast milk reduces the risk for your baby in the development of allergies and insulin dependant diabetes. It is less work and is always the right temperature and consistency.
Breastfeeding also offers health benefits for your partner with a reduced risk of post menopausal breast cancer, ovarian cancer and osteoporosis.
Most mothers make a decision about how they will feed their baby before they become pregnant or during pregnancy, and you are a very influential person in that decision. There is a clear body of evidence that where a couple have made a joint commitment to breastfeed their baby before birth, the mother is more likely to successfully establish and maintain breastfeeding.
If your partner is expressing any reservations about breastfeeding, discuss her concerns to help her make an informed choice based on accurate information. If your partner expresses any doubt whatsoever about her ability to breastfeed or her supply of milk, you can help by telling her how well she's doing, reminding her of the benefits of breastfeeding, and by helping her find accurate and complete information to remove any doubt. Don’t underestimate your ability to help your partner to successfully breastfeed.
Your midwife, obstetrician, antenatal classes and the Australian Breastfeeding Association are excellent resources in this regard.
Sex
Following birth, the hormone levels in a woman’s body signal it to produce and release milk and contract the uterus. As a result of the changes and adjustments birth brings, your partner may temporarily lose interest in sexual intercourse. This can happen whether the woman is breastfeeding or formula feeding. Many men become closely involved in the breastfeeding experience and spend time lying or sitting near the mother, sharing the enjoyment of a baby breastfeeding.
The natural slipperiness of the vagina may not be present at the beginning of the breastfeeding experience; there are products available eg. KY jelly—which helps lubricate the vagina. Be sensitive to your partners needs as she gains confidence in breastfeeding and recovers from the birth and interrupted sleep. There are other ways of showing your love—a kiss, a hug, holding hands etc. Take things slowly and talk to one another.
Mater acknowledges consumer consultation in the development of this patient information.
Mater Doc Num: PI-CLN-430067
Last modified 23/1/2020.
Consumers were consulted in the development of this patient information.
Last consumer engagement date: 19/1/2014
For further translated health information, you can visit healthtranslations.vic.gov.au/ supported by the Victorian Department of Health and Human Services that offers a range of patient information in multiple languages.