Breast Cancer and Wide Excision
Welcome
At Mater Hospital Brisbane, we understand that being hospital can be a very stressful experience. In keeping with our Mission to offer compassionate, quality care that promotes dignity whilst responding to patients' needs, this booklet aims to alleviate some of your concerns. It explains the general day to day events that may occur during your visit and the things to expect when you are discharged from the hospital.
It is, however, only a guideline as each person may require differing treatments.
If you have any questions about your treatment please speak to your doctor or nurse. Our pastoral care team offers a caring support network to all patients. The dedicated members of this team will visit you during your stay and are available at your request to discuss any anxieties or problems that you may have.
Breast cancer
You have recently been diagnosed with breast cancer.
What are the principles of breast cancer treatment?
- Treat the breast in which the cancer has developed.
- Assess the axillary lymph nodes and treat as required.
- Treat the rest of the body if there is any significant risk that cancer cells may have spread.
Breast conservation treatment
Breast conservation treatment is defined as the excision of the primary breast tumour and adjacent breast tissue. If not enough of the normal tissue is removed you will be required to have another operation called a re-excision. Some of the lymph nodes in the armpit (axilla) are also removed during breast conservation surgery.
Breast conserving surgery also is commonly referred to as lumpectomy, partial mastectomy, wide local excision and quadrantectomy.
There can be a cosmetic deformity from where the tumour is removed. This takes the form of a minor indentation and slight distortion of the nipple on that side. Usually there is no need to change bra size from the removal of the tumour from the breast.
After your recovery from this operation, (usually one month), the remaining breast tissue is treated with a course of radiotherapy. Approximately 80 per cent of breast cancers will be able to be managed this way.
A mastectomy will not be performed at the time of the above operation if a breast conservation procedure has been decided on by you and your doctor. Should the need for this surgery be required, it will be discussed during further consultation with your doctor.
Mastectomy
Twenty per cent of breast cancers will require the breast to be treated by mastectomy—removal of the breast tissue including the nipple. This will be determined pre-operatively.
It is recommended if:
- the tumour is in more than one part of the breast
- the tumour is large, (greater than four centimetres in diameter)
- there is a strong desire not to have post operative radiotherapy
- this would be inconvenient (if you live away from the east coast)
- this is the woman's personal choice.
Sometimes where mastectomy is recommended, a breast reconstruction could either be performed at the same time or at a later date.
The lymphatic system
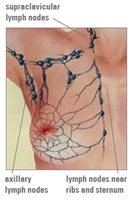 The lymphatic system is a network of glands connected throughout the body by tiny vessels called lymph vessels. Lymph vessels contain lymph. Lymph is a yellow fluid with cells called lymphocytes. Lymphocytes help fight disease. The lymph flows through the lymphatic system and eventually drains into veins. This system helps to get rid of waste products from the body.
The lymphatic system is a network of glands connected throughout the body by tiny vessels called lymph vessels. Lymph vessels contain lymph. Lymph is a yellow fluid with cells called lymphocytes. Lymphocytes help fight disease. The lymph flows through the lymphatic system and eventually drains into veins. This system helps to get rid of waste products from the body.
The diagram to the right displays the lymph drainage of the breast.
Why lymph nodes are removed
Lymph nodes under the arm can be the first site where breast cancer spreads. The only way to determine whether breast cancer has spread to the lymph nodes is to remove and analyse them. Lymph node removal is performed for individuals who have invasive breast cancer, whether they have breast conservation or mastectomy. Information from lymph node analysis contributes to determining any further treatment if required. It also removes any cancerous glands to reduce the risk of the cancer reoccurring in the armpit.
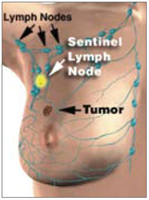 Sentinel lymph node biopsy is a technique of mapping the very first lymph node/s which would be encountered in the lymph node basin draining away from the breast cancer. It is performed by injecting blue dye around the tumour or under the nipple. The dye quickly moves into the lymph vessels and aims to stain the sentinel nodes blue. This helps the surgeon identify them. The dye stains the urine blue or green for one day or so after the surgery. It also stains the breast tissue. This gradually fades over time.
Sentinel lymph node biopsy is a technique of mapping the very first lymph node/s which would be encountered in the lymph node basin draining away from the breast cancer. It is performed by injecting blue dye around the tumour or under the nipple. The dye quickly moves into the lymph vessels and aims to stain the sentinel nodes blue. This helps the surgeon identify them. The dye stains the urine blue or green for one day or so after the surgery. It also stains the breast tissue. This gradually fades over time.
Sentinel lymph node biopsy can also be performed by injecting a small amount of radioactivity (approximately 1/20th the dose of a bone scan) around the tumour and then detecting the first lymph node encountered using a hand held Geiger counter. You can speak to your surgeon regarding the performance of this test.
If the sentinel node/s contains cancer cells or the cancer is already known to have spread to the lymph nodes (e.g. palpable or seen on ultrasound) a full lymph node clearance of the axilla will be recommended.
Within a week of surgery, provided that no further surgery needs to be performed, consultation will be made with a radiation oncologist and a medical oncologist to plan the next phase of your treatment.
Recovery
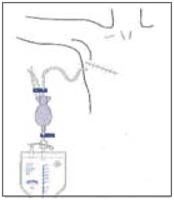 Most patients are sufficiently pain free to be able to return home within a day or two of surgery. If a full lymph node clearance has been performed, a fine drain is inserted into the armpit. This needs to stay in place until the drainage is less than 50mls of fluid on two consecutive days, or less than 30mls on one day. Patients are able to go home with this drain in place although the drain is sometimes removed prior to discharge from hospital. Should you be discharged with your drain in place, the nursing staff will teach you how to manage the drain at home. The nursing staff will provide you with contact numbers should you need assistance with your drain after hours.
Most patients are sufficiently pain free to be able to return home within a day or two of surgery. If a full lymph node clearance has been performed, a fine drain is inserted into the armpit. This needs to stay in place until the drainage is less than 50mls of fluid on two consecutive days, or less than 30mls on one day. Patients are able to go home with this drain in place although the drain is sometimes removed prior to discharge from hospital. Should you be discharged with your drain in place, the nursing staff will teach you how to manage the drain at home. The nursing staff will provide you with contact numbers should you need assistance with your drain after hours.
Post operative arm exercises/physiotherapy
You will be visited by a physiotherapist who will discuss the care of your arm and demonstrate exercises to assist in regaining full range of movement of your arm in the future.
You will be provided with a booklet which will describe these exercises in further detail.
Side effects of lymph node surgery
During the removal of the lymph nodes a nerve can be stretched. Due to this, 90 per cent of women will have a degree of numbness on the inside of their arm. As well as pain on moving the shoulder where the lymph nodes have been removed, there is sometimes limitation of movement due to scarring in the armpit.
Lymphoedema (swelling of the arm) may develop in approximately five per cent of patients undergoing removal of the lymph nodes. The risk of lymphoedema can be reduced by carefully avoiding the triggering factors as explained in the physiotherapy booklet. Lymphoedema would be detected at follow up visits or you may notice it yourself. All of your cancer specialists will check for its presence within the first year after surgery. This can be treated initially by elevation, massage techniques and sometimes by bandaging. Occasionally, patients will need to wear compressive garments to prevent it getting any worse.
Sometimes the lymphatic fluid which has been draining builds up under the wound after removal of the drain from the armpit. This fluid is called a seroma. If it becomes symptomatic the wound will need to be aspirated.
Risks and complications
Apart from those mentioned above, there is approximately a two to three per cent chance of bleeding or developing an infection requiring a return to the operating theatre.
The risks associated with surgery are those mainly related to the armpit operation, where the patients may have numbness or altered sensation on the inner aspect of the arm.
Sometimes, if the operation is close to the nipple, nipple sensation will be impaired permanently.
Treatment of the rest of the body—adjuvant or systemic therapy
Radiotherapy
Radiotherapy is a treatment using radiation to destroy cancer cells. A small dose is given and takes less than five minutes each working day for six weeks. The commencement of this can be delayed for up to three months after the surgery or after any chemotherapy has finished. However once begun, it is preferable not to interrupt this treatment. Sometimes radiotherapy will be necessary following a mastectomy, especially if the cancer is large (greater than five centimetres) or more than three lymph nodes are involved with cancer. The prime reason radiotherapy is given is to reduce the chance of the cancer returning in the breast. There is initially some swelling in the breast while undergoing radiotherapy, though most of this will completely settle within a year of surgery.
Hormone therapy—Tamoxifen/Arimidex/Femara
Tamoxifen is the most common hormone treatment used today. It works by blocking the stimulating effect of oestrogen on breast cancer cells. Arimidex and Femara work by lowering oestrogen levels for post menopausal women.
Like chemotherapy, hormone therapy is systemic—that is, it works throughout the body.
In cases where the cancer is sensitive to hormones, studies have found that hormone therapy should be used for five years following surgery.
Chemotherapy
Chemotherapy will be considered as a form of systemic treatment. If you need to have chemotherapy, this will be fully explained by your medical oncologist or oncology nurse. This treatment will be given two or three weeks apart extending over three—six months. This will usually take place before your radiotherapy treatment.
It is helpful to attend a chemotherapy education session. Recently, great strides have been made in cancer chemotherapy. New, more effective combinations have been developed. Side effects such as nausea are now better controlled by new anti-nausea drugs.
Neither chemotherapy nor radiotherapy will commence in the immediate fortnight following surgery while your wounds are healing.
Herceptin
Apart from hormone and chemotherapy a sophisticated biological agent, Herceptin has also been shown effective in preventing cancer recurrence in susceptible patients, notably those with a cancer that is HER2 positive (up to one quarter of cancers).
Staging investigations
Bone scans, chest x-rays, and liver scans are tests which may be requested by your doctor, following surgery, to determine if the cancer was contained within the breast.
Follow-up after surgery
At each appointment a clinical examination will be performed. If you have noticed any swelling of your arm or breast, notify your breast care nurse.
If for any reason you have not had an appointment with your doctor, contact your surgeon, medical oncologist or radiation oncologist.
Mammography
A mammogram will be performed one year after surgery and then annually. The arrangements for the mammogram will be made at the previous appointment. If you have not had a mammogram within the last 12 months, contact your doctor.
Breast health
"Being breast aware is part of general awareness. Being breast aware means learning how your breasts look and feel. It is important to know what is normal for you. Everyone is different and as you go through the different stages of your lives, your breasts are continually changing."
For further information, visit http://www.breastcancer.org.au/about-breast-cancer/risk-factors/being-breast-aware.aspx for Breast Health—Being Breast Aware.
Keeping your records
The My Journey kit has been developed for you by women who have had breast cancer.
The kit contains:
- an appointment diary with business card record section
- a book of practical tips, useful contacts and resources.
To order your free kit call 1300 785 562 and leave your details on the answering machine. It will be delivered to your home within five to seven days of your call.
Managing your friends and colleagues
The brochure Helping a Friend or Colleague with Breast Cancer is about women who have had breast cancer sharing the things they found helpful and unhelpful. Call 1800 500 258 for a copy or download it directly from the internet at www.bcna.org.au/helping_a_friend_or_colleague_with_breast_cancer
Support groups
There are many programs and support groups that offer support for women with breast cancer.
It is very important to share your concerns with your surgeon, breast care nurse and treatment team. Information about the following programs is available from your breast care nurse. All programs are free.
Look Good...Feel Better Program
This workshop is available to men and women with cancer. In a relaxed and friendly workshop environment you will learn how to manage the visual changes that may occur to your skin as a result of treatment including wig and turban demonstrations.
Workshops last for approximately two hours and you are welcome to bring a support person. This program runs nationally.
For Look Good...Feel Better program contact Choice—Monday to Friday from 8.30 am to 5 pm.
Free call: 1800 657 960
Website: www.lgfb.org.au/
Young Women's Network
This network provides information and support for younger women with breast cancer. Meetings are held monthly. Conducted by Cancer Council Queensland. Statewide telephone contact and mailing services available.
Contact number: 13 11 20
Email for general enquiries: info@cancerqld.org.au
Email for help: helpline@cancerqld.org.au
Website: www.cancerqld.org.au
Breast Cancer Matters
This is an educational and support program for women and their families. The program is designed to provide information about:
- breast cancer
- breast cancer treatments
- stress management
- self-image and relationships.
It also provides women with an opportunity to share experiences. This program is conducted regularly by Cancer Council Queensland and other centres.
YWCA Encore program
Encore is an exercise program designed specifically for women who have experienced mastectomy, lumpectomy or breast reconstruction surgery at any time in their lives. Based around floor and pool exercises and relaxation techniques, it is safe, fun and therapeutic. This program is available at a number of delegated venues.
For more information contact:
Contact number 1800 305 150
Website: www.ywcaencore.org.au
Counselling services
- Mater Hospital Brisbane–contact your breast care nurse who can refer you to counselling professionals.
- Cancer Council Queensland–phone 13 11 20
Contact hours: Monday to Friday, 8 am to 8 pm. Both a telephone service and a face to face counselling service is available to you.
Rural patients
Accommodation information for patients from rural areas is available from preadmission.
Resources
For you
Cancer Council Queensland
Cancer Australia (Home)
Cancer Australia (Breast Health)
New South Wales Cancer Council
Oncolink (U.S.A.)
National Cancer Institute (U.S.A.)
For partners
Cancer Australia (Boys do cry)
Helping teenagers
Cancer Australia (My parents cancer)
Young children
What’s happening to my mummy book available from the Breast Care Unit or Cancer Council Queensland by calling 13 11 20
chicks in pink
“chicks in pink” supports Mater in its care for women with Breast Cancer. In targeting “chicks” of all ages its aim is to become “the thinking chicks charity of choice” and increase community awareness of breast cancer through fun and educational fundraising events.
Website: www.chicksinpink.com
Wide excision / axillary dissection patient information guide
Expected length of hospital stay
The expected length of hospital stay is overnight.
After your operation
- You will stay in recovery within the theatre suite, after the operation, while you waken from the anaesthetic before returning to your room in the post-operative unit.
- Your nurse will take frequent observations of your vital signs (e.g. pulse, respirations, temperature and blood pressure) and wound, dressings and drain/s for several hours after the surgery. These will become less frequent as you recover but remain regular until you leave hospital. It is important that your blood pressure is not taken on your operative side.
- You will be resting in bed immediately after your surgery. When you are ready to get out of bed for the first time following your surgery it is important that you have assistance.
The following exercises help prevent complications suchas chest infections and blood clots in your legs. You should do these every hour that you are awake while resting in bed.
Breathing exercises: take five long and slow deep breaths. Each breath should be deeper than the previous breath. Think about getting the air to the very bottom of your lungs.
Circulation exercises: firmly move your ankles up and down to stretch and contract your calf muscles.
- When you have recovered from your anaesthetic you will be reminded to do the deep breathing and coughing exercises while resting in best.
- About four hours after you return to the ward, your nurse will assist you to have a wash.
- You may have small amounts of water or ice to suck, then progress from fluids to a normal diet as tolerated.
- If you have pain or nausea, please tell your nurse as there are medications which can be given to relieve this. It is important to be comfortable.
- The drip (IV) is necessary to maintain your fluid intake. This will be removed when you are tolerating adequate amounts of oral fluids.
- You may have a drain in place under your arm where the lymph nodes have been removed. Your underarm drain will remain in place until the amount of drainage decreases sufficiently for it to be removed. The length of time this drain remains in varies from person to person. It is possible that you will be going home with the drain still in. If this is the case the nursing staff will give you the necessary education to allow you to confidently manage the drain at home. You will also have a second drain in place at the wound site. An additional booklet that demonstrates a step by step guide to manage the drain will be given to you. This drain may be or may not be removed before you go home.
- Your physiotherapist will visit either on the day of surgery or the day following surgery to explain exercises that will help with your post-operative recovery and provide you with additional information to follow.
- Do not be alarmed if your skin colour, urine and bowel movements have a bluish tinge. This is due to the blue dye that is used during the operation.
The day you go home
You will be ready to go home when:
- you are mobilising to the same level as you were prior to your admission
- you are maintaining adequate oral intake
- your pain is controlled with oral analgesia
- you have received education regarding your postoperative arm exercises/physiotherapy
- you have received explanations regarding your post-operative care by your breast care nurse
- you have received your post-operative appointments
- your discharge plan has been completed.
What to expect
Pain management
You can expect some discomfort from your wound. It may be necessary to take some simple oral analgesia as prescribed by your doctor. You will find that you will need this analgesia for the first week after your operation. After this time you may have some discomfort/pain but may not need analgesia. Your pain should continue to decrease over the following week.
Wound management
Your wound may be slightly red, raised and you may have some bruising. This is part of the normal healing process and should subside within two to three weeks of your operation. A waterproof dressing will be in place and you can shower normally. Up until three months following surgery, your wound may become thickened. This is part of the normal healing process.
Exercises
You can expect some restrictions in the range of movement on your operated side. Please continue the exercises the physiotherapist gave to you. You can expect to have full shoulder movement by six weeks. If you have any problems with your exercises, please contact your breast care nurse on 07 3163 8111 (pager: 0732 or 4732).
Nutrition and rest
You may feel tired for a few days. Remember, you have had an operation so get plenty of rest, and maintain a good nutritious diet and adequate fluid intake. You can increase your daily activity as you feel stronger. After a few days at home, start walking short distances (e.g. five to ten minutes) twice a day.
Drain and dressing
You may be discharged from hospital to home with a drain in place. Your breast care nurse will provide you with education to care for your drain and dressing.
Long-term follow up plan
| Follow-up period |
Frequency of follow-up visits |
| Tests |
|
|
First year
|
Three monthly
|
|
Second to fifth years
|
Six monthly
|
|
Fifth year
|
Yearly (you may be discharged back to Breast Screen or your local GP at this time)
|
|
Mammogram
|
Yearly
|
|
Ultrasound
|
Yearly if diagnostic mammogram was negative when < 35 years
|
At each appointment a clinical examination will be performed. If you have noticed any swelling of your arm or breast, notify your breast care nurse.
Please contact
Mater Hospital Brisbane Day Procedure Unit—07 3163 8324, Mater Hospital Brisbane Emergency Department—07 3163 8111, or your GP if any of the following occur after discharge:
- your wound becomes red or inflamed or discharge increases
- you develop a fever (temperature above 38 degrees Celsius)
- you have pain that is not relieved by simple analgesia.
Acknowledgments
Staff of Mater Hospital Brisbane, Raymond Terrace, South Brisbane, Q 4101
Contact details
Mater Hospital Brisbane
Raymond Terrace,
South Brisbane Q 4101
Website: www.mater.org.au
© 2012 Mater Misericordiae Ltd. ACN 096 708 922.
Mater acknowledges consumer consultation in the development of this patient information.
Mater Doc Num: PI-CLN420007
Last modified 17/3/2020.
Consumers were consulted in the development of this patient information.
Last consumer engagement date: 08/11/2015
For further translated health information, you can visit healthtranslations.vic.gov.au/ supported by the Victorian Department of Health and Human Services that offers a range of patient information in multiple languages.